Breast Reconstruction Newport Beach, CA.
Breast Reconstruction
Breast reconstruction is one of the most challenging aspects of Plastic & Reconstructive surgery. There are many different variables that need to be considered and addressed to either maximize the aesthetic outcome of the breast reconstruction or to progress the breast cancer patient on to their next modality of oncologic therapy. Having a breast cancer diagnosis can be emotional, confusing, and understanding the treatment regimen can be difficult. It is important to keep things simple. I have been performing breast reconstruction for over 20 years. I perform oncoplastic reconstruction for lumpectomy and mastectomy breast reconstruction including DIEP flaps and other forms of autologous reconstruction. I hope the information on this page and in the blogs can help you understand breast cancer treatment and breast cancer reconstruction better.
Lumpectomy
Often the first step in breast reconstruction is to determine if you are going to have a lumpectomy or a mastectomy to treat your breast cancer. In general, a lumpectomy can safely be performed and the aesthetic outcome excellent if you have a tumor that is relatively small in proportion to a larger breast. If you have a lumpectomy and have a breast cancer, you will need radiation therapy after your lumpectomy to complete the oncologic treatment. If you have ductal carcinoma in situ (DCIS), which is a “pre-cancer” there may be a possibility that you do not need radiation after lumpectomy depending upon the grade of DCIS, the size of DCIS, your age, and the margins. In some situations, you may be able to have radiation therapy delivered intra-operatively at the time of your lumpectomy. Depending upon the type of cancer and status of your lymph nodes you may need chemotherapy prior to your breast cancer surgery or after your breast cancer surgery. Navigating the oncologic treatment of breast cancer and trying to understand decisions to maximize your aesthetic result can be extremely confusing. This is confounded by the fact that a breast cancer diagnosis in itself can be extremely confusing. What is important is to just keep things simple as you go through the process. We understand the process is confusing. After you have a consultation with us, you are always welcome to call the office if you have questions and you are always welcome to come back to the office for a second consultation if there are more questions. Over time, as you meet, speak, and listen to your oncologic surgeon, your medical oncologist, your radiation oncologist, and your plastic surgeon you will hear similar words and terms over and over again and eventually the process will make sense.
If you would like to learn more about lumpectomy and oncoplastic reconstruction of lumpectomy defects, please click on the banner below and you will be directed to the breast reconstruction blog. In the blog section you may encounter patients with anatomy and with surgical treatment plans similar to you. In some blogs the patients will be in early stages of healing and in other blogs the patients will be in later stages of healing. This is designed to help you understand breast cancer surgery and breast cancer reconstruction. After your lumpectomy and oncoplastic reconstruction consultation, we will provide you with the post-operative recovery pathway in an easy-to-follow grid format.
Click Here to View the Breast Reconstruction Blogs
Mastectomy
There are many different ways that a plastic and reconstructive surgeon is able to reconstruct the breast after a mastectomy. Which breast reconstruction method you choose or decide upon depends upon factors such as your general health, history of radiation to the mastectomy site, smoking history, need for chemotherapy post mastectomy and prior operations on the breast or in the abdomen. Below are some of the more common types of breast reconstruction:
- TRAM Flap Breast Reconstruction Methods:
- Pedicled TRAM flap
- Free TRAM flap
- Muscle sparing free TRAM flap
- DIEP Flap Reconstruction
- Implant Breast Reconstruction
- Tissue Expander/Breast Implant Reconstruction
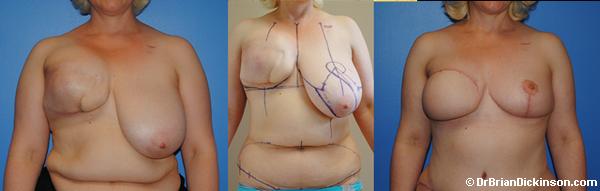
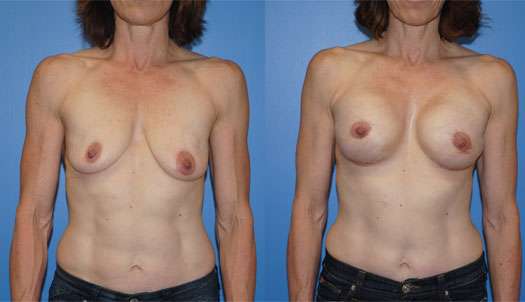
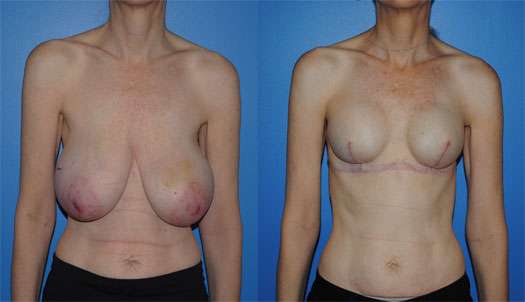
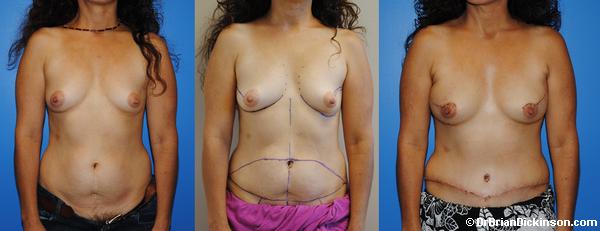
Of the different types of patients and clinical problems we encounter in consultation, the breast reconstruction consultation is always the most dynamic. I have tried to make this consultation as linear as possible, but it always includes both the patient and I standing up/sitting down, me drawing on you and you asking questions about what I am drawing on you. While I try to answer as many of your questions as I can, there are several concepts or pre- and post-operative sequences that I will need to convey to you during your consultation. These include nutrition, hyperbaric oxygen, radiation, recovery, complications, etc. Describing each of these for both the lumpectomy and mastectomy pathways or options can take time. I will do my best to listen to your concerns and questions. Many of your questions will be answered in the descriptions we explain to you in the consultation.
After the consultation and prior to your surgery we will provide you with a grid that has the post-operative instructions in a neat pathway format for you to follow after your surgery. This is designed to help alleviate any anxiety and make the process as simple as possible for you. If you have questions in the post-operative period, however, please do not hesitate to call. I would rather we communicate and answer your question than to have you do something you should not have done.
When the breast has been removed for cancer and the remaining skin on the chest has been radiated and is also unamenable to implant based reconstruction, my preferred method of breast reconstruction is to use tissue from the lower abdomen. The DIEP flap allows the reconstructive surgeon the opportunity to utilize the skin and fat from the lower abdomen while attempting to spare muscle. The end result is that the mastectomy defect can be reconstructed, and the patient can have the lower abdomen contoured.
Operations such as these are variations of a TRAM flap breast reconstruction. TRAM stands for Transverse Rectus Abdominus Myocutaneous flap. The blood supply to the skin and fat on the lower abdomen is derived from blood vessels that traverse through the muscles of the abdomen.
The skin and fat of the lower abdomen can be transferred to the site of your mastectomy. This can be done with a TRAM flap where the skin, fat, and muscle remain connected to an original blood supply. There are varying degrees of modification of the donor site in breast reconstruction. The DIEP flap is a variation where muscle is spared from the lower abdomen with the intent of transferring only the skin and fat from the lower abdomen and minimizing the donor site.
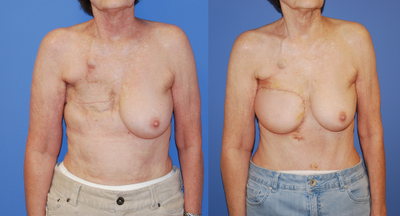
This type of DIEP flap breast reconstruction procedure can be performed in Newport Beach, CA. The procedure requires a general anesthetic and an inpatient stay in the hospital. In some patients who previously had multiple abdominal operations, a CT-angiogram can be helpful in determining the integrity of vessels as well as in determining which flap may be an appropriate option for the patient such as TRAM, TRAM flap with pre-delay procedure, free TRAM, DIEP, or SIEA.
Depending upon your body type or body habitus, you may or may not be a candidate for an autologous reconstruction. In patients with a body mass index that is too low < 18, there may not be enough tissue on the abdomen to reconstruct both or even one breast. In patients with a body mass index that is too high > 30 you may also not be a candidate for flap reconstruction as the risk of complications can be more significant. In patients who are committed to weight loss, the staged fashion of breast reconstruction can be a unique opportunity for weight loss and cancer risk reduction.
For more information on autologous breast reduction please read our publication here:
For any additional questions and answers, you may review the breast reconstruction blog that is present on this website.
From the Blog
Bilateral DIEP Flap Reconstruction and Prior Radiation
Deep Inferior Epigastric Artery Perforator (DIEP) flaps are often a great choice when reconstructing the…
Read MoreAutologous Breast Reconstruction. DIEP Flaps. Second Stage Procedures
Autologous breast reconstruction involves reconstructing the breast following mastectomy with the patient's own body tissues.…
Read MoreDIEP Flap Breast Reconstruction, to Replace Medial Breast Skin Following Mastectomy
Breast reconstruction in the radiated patient is different than in patients who have not received…
Read More