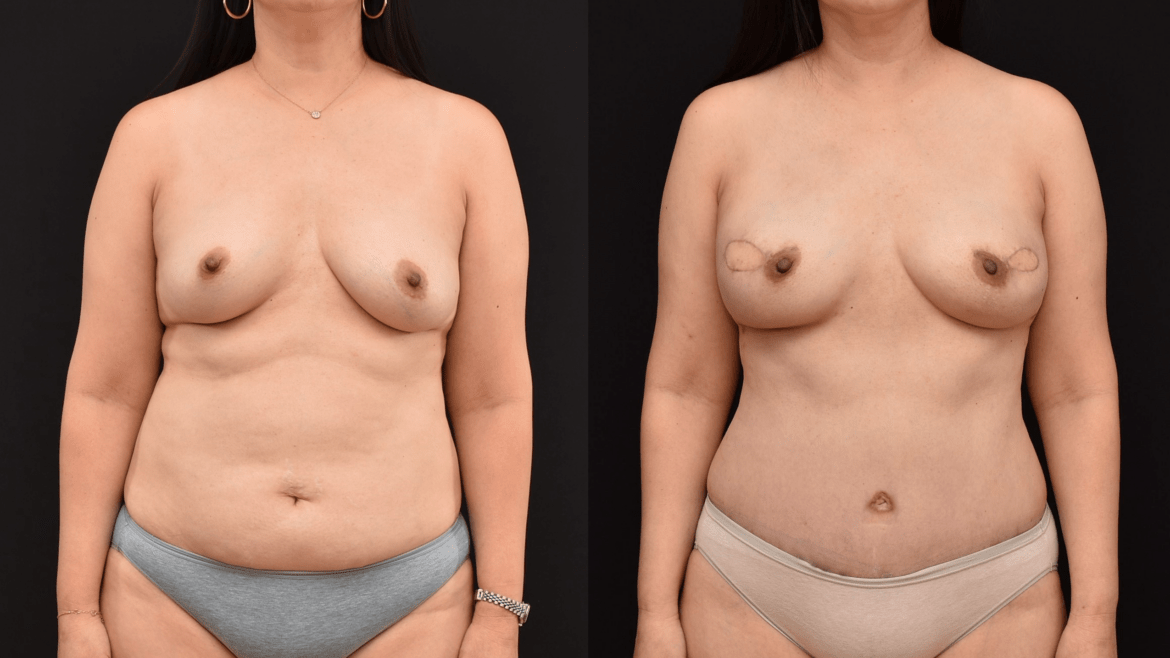
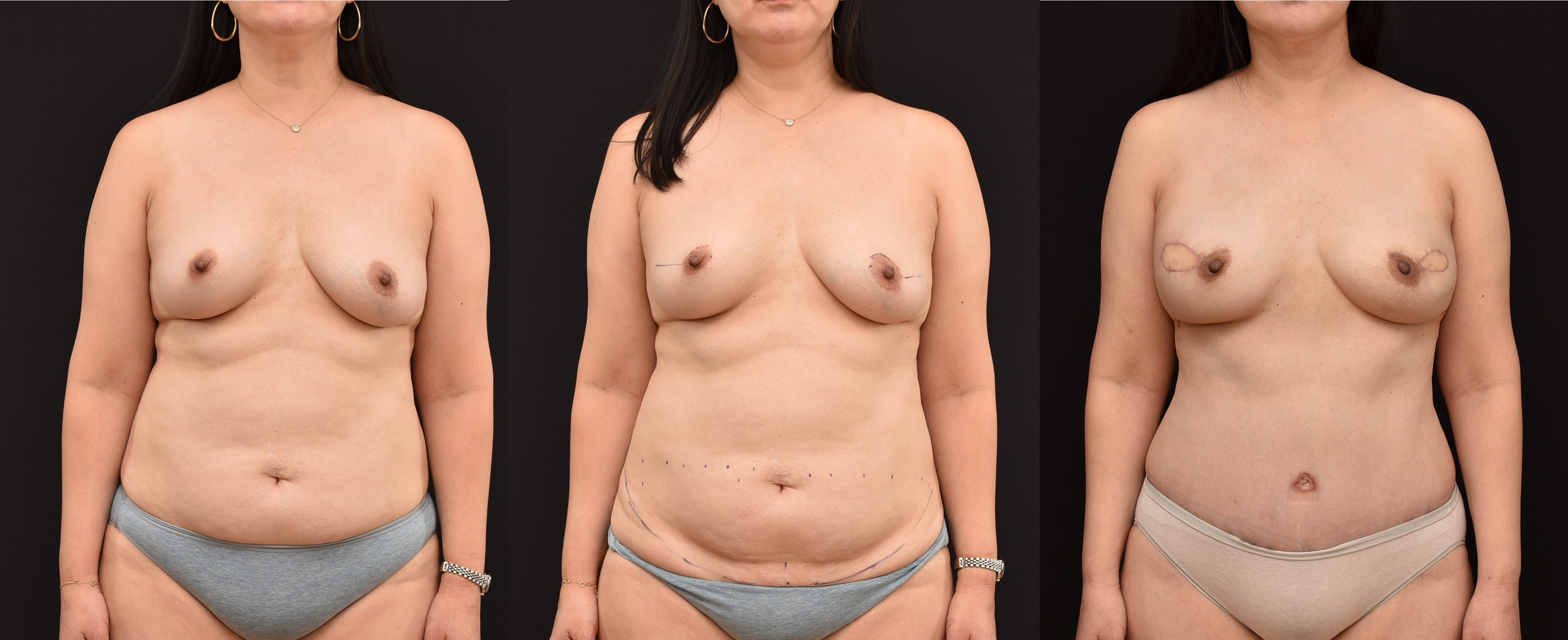
Breast reconstruction following mastectomy can be performed with tissue expanders and implants. In some cases, patients do not want to have their breast reconstructed with implants and we can use the skin and fat from the abdomen to reconstruct the breast. In some patients the DIEP flap can be completed at the time of the mastectomy depending upon the size of their cancer, their body habitus as well as any comorbidities. There are different types of skin patterns that can be used to gain access to perform the mastectomy. The superior periareolar approach with a lateral extension allows the nipple areola complex to remain alive on a random skin pattern from the inferior aspect of the breast.
The mastectomy is performed and the breast is removed. The third interspace is identified and the cartilaginous portion of the third rib is removed to gain access to the internal mammary artery and vein. Once the internal mammary artery and vein are identified, the skin and fat from the lower abdomen are dissected and the blood vessel supplying the skin and fat is dissected free. The skin and fat are then brought up to the chest as a composite microvascular soft tissue transfer and the deep inferior epigastric artery and vein are attached to the internal mammary artery and vein. A portion of the abdominal skin is kept visible on the breast so that the blood supply of the flap can be monitored. This skin paddle is then removed if desired at a second stage. In some patients, depending upon the size of the skin paddle, the skin paddle may contribute to the overall shape of the breast. Scars that are recent (< 1 year) tend to be red in color. The redness will fade over time and become significantly lighter.